LISTEN TO STORY
WATCH STORY
By: Isuru Parakrama
May 04, Colombo (LNW): The recent hantavirus scare linked to the cruise vessel MV Hondius has exposed a familiar but uncomfortable truth: the world remains dangerously reactive, rather than prepared, when confronting zoonotic diseases. While global authorities have downplayed the immediate risk, the outbreak underscores a deeper structural vulnerability—one that countries like Sri Lanka can ill afford to ignore.
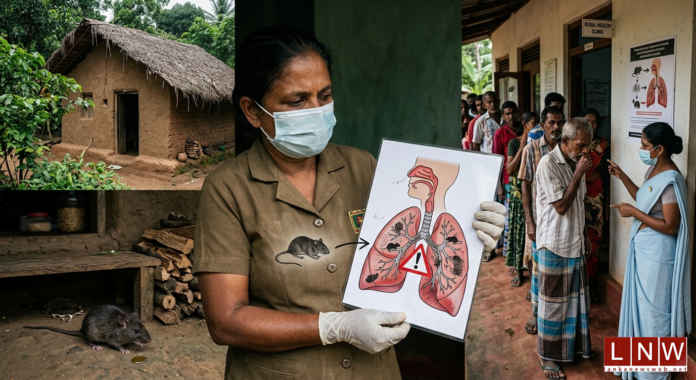
Hantavirus is not new, nor is it particularly mysterious. It is a rodent-borne zoonotic virus group, transmitted primarily through inhalation of aerosolised particles from rodent urine, droppings, or saliva. Less commonly, infection may occur through contaminated food or bites.
Yet despite its well-established transmission pathways, it remains a high-consequence pathogen due to its capacity to escalate rapidly from flu-like symptoms to severe respiratory distress, shock, and death.
A Disease Defined by Severity, Not Spread
Unlike Covid-19, hantavirus is not typically a mass-transmission pandemic agent. However, this distinction should not breed complacency. The pulmonary syndrome variant, common in the Americas, carries significant lethality, while the haemorrhagic fever with renal syndrome variant affects Asia and Europe on a large scale—estimated at around 150,000 cases annually.
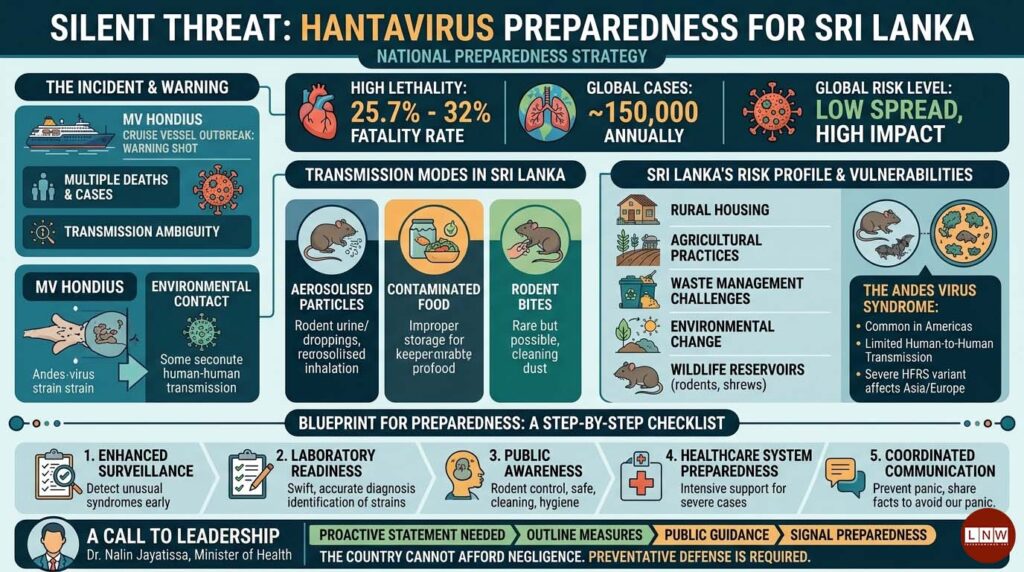
The numbers from 2025 alone are sobering. Across the Americas, 229 confirmed cases resulted in 59 deaths, translating to a fatality rate of 25.7 per cent. Argentina, the epicentre in the region, reported 66 cases and 21 deaths—a striking 32 per cent lethality rate, higher than previous years.
This is not a mild disease. There is no widely available antiviral cure. Treatment is largely supportive, meaning outcomes depend heavily on early detection, clinical capacity, and overall health system readiness.
The MV Hondius Incident: A Warning Shot
The unfolding situation aboard the MV Hondius has transformed hantavirus from a regional concern into a global talking point. With multiple deaths, at least one confirmed case, and several suspected infections, the incident illustrates how quickly uncertainty can spiral in confined environments.
What makes this outbreak particularly unsettling is the ambiguity surrounding transmission. Hantavirus is usually not spread between humans. However, the Andes virus strain—prevalent in parts of South America—has demonstrated limited human-to-human transmission under close and prolonged exposure.
This nuance matters. It shifts hantavirus from being purely an environmental hazard to a potential, albeit limited, interpersonal threat. Even if the global risk remains low, as the World Health Organisation suggests, the implications for surveillance and containment are significant.
Why Sri Lanka Cannot Afford Indifference
Sri Lanka’s geographic and socio-economic realities make it vulnerable to zoonotic spillovers. Rural housing conditions, agricultural practices, and waste management challenges create ideal conditions for rodent-human interaction—the primary driver of hantavirus transmission.
Environmental change further compounds the risk. As ecosystems shift and human activity encroaches into wildlife habitats, opportunities for spillover increase. Hantavirus, deeply rooted in wildlife reservoirs such as rodents, shrews, and even bats, cannot be eradicated in the conventional sense.
The lesson is clear: prevention is not optional—it is the only viable defence.

A Blueprint for Preparedness
If hantavirus were to reach Sri Lanka’s borders, the response must be immediate and multi-layered. The Pan American Health Organisation has already outlined the essential pillars: strengthened surveillance, rapid laboratory diagnosis, effective clinical management, and intersectoral risk reduction.
For Sri Lanka, this translates into:
- Enhanced surveillance systems capable of detecting unusual respiratory or renal syndromes early.
- Laboratory readiness to identify hantavirus strains swiftly and accurately.
- Public awareness campaigns focused on rodent control, safe cleaning practices, and environmental hygiene.
- Healthcare system preparedness, particularly in managing severe respiratory cases requiring intensive support.
Equally critical is the need for coordinated communication. Panic thrives in silence, and misinformation fills the void left by indecision.
A Call to Leadership
Hantavirus is often described as a “low-risk” global threat. That characterisation, while technically accurate, is dangerously misleading. The true risk lies not in widespread transmission, but in high fatality, limited treatment options, and persistent ecological reservoirs.
It is, in essence, a silent threat—one that does not overwhelm systems through volume, but through severity.
This is where political accountability must come into sharp focus. Sri Lanka cannot wait for an outbreak to begin drafting its response. The country’s Minister of Health, Dr. Nalinda Jayatissa, must proactively address the nation on this issue.
A clear, evidence-based statement outlining preparedness measures, potential risks, and public guidance would not only reassure citizens but also signal that the government is not sleepwalking into the next public health crisis.
The absence of such leadership would be more than an oversight—it would be negligence. The world has already learned this lesson the hard way. There is little excuse for repeating it.